Caregiver Support in Fibrodysplasia Ossificans Progressiva
Mona Al Mukaddam1, Kin Cheung2, Sammi Kile3, Michelle Davis3, Frederick S. Kaplan1,4 Robert J. Pignolo5*
1Departments of Medicine, Orthopaedic Surgery, and The Center for Research in FOP and Related Disorders, The Perelman School of Medicine, the University of Pennsylvania, Philadelphia, PA, USA
2BioSAS Consulting, Inc., Wellesley, Massachusetts, USA
3International FOP Association (IFOPA), North Kansas City, Missouri, USA
4Isaac & Rose Nassau Professor of Orthopaedic Molecular Medicine
5Chair, Geriatric Medicine & Gerontology, Robert and Arlene Kogod Professor of Geriatric Medicine, Mayo Clinic College of Medicine, Mayo Clinic, Rochester, MN, USA
Abstract
Background:Fibrodysplasia ossificans progressiva (FOP) is an ultra-rare disease characterized by malformed great toes and progressive heterotopic ossification (HO) in soft tissues. Current standard-of-care is aimed at palliation of symptoms; there are no currently approved therapies to prevent HO. Recurrent episodes of HO starting in early life lead to cumulative disability, severe functional limitations, and shortened life span. Most individuals require assistive devices and extensive caregiver support before the second decade of life. Caregiver support is thought to be high, but the timing and extent of caregiver support in FOP has not been formally assessed. Methods: Using data from the International FOP Association (IFOPA) Global Registry on 299 patients (median age 21 years; range 0.1 to 78 years) from 54 countries, we characterized the extent of caregiver support by assessing the number of part-time and full-time caregivers and school aides reported by participants, based on age. Results: Over 50% of FOP Registry respondents reported a need for part-time or full-time home personal care attendants. The percentage of individuals who reported a requirement for bathing attendants and part- or full-time home personal care attendants increased with age (>1 part-time or full-time caregiver exceeded 30% for individuals >15 years of age), as did the number of part-time or full-time attendants. Support from school aides peaked between 9 and 15 years of age. Conclusion: Caregiver support in FOP is high in terms of time and amount of support needed, increases rapidly with age, and is substantial by the second decade of life. These findings highlight the urgent need for transformative treatments that will preserve the independence of individuals with FOP.
Introduction
Fibrodysplasia ossificans progressiva (FOP; OMIM #135100) is an ultra-rare and progressively disabling disorder with a prevalence between 0.5 and 1.4 per million1,2. FOP is characterized by episodic flare-ups and irreversible heterotopic ossification (HO) in muscles, tendons, ligaments, fascia, and aponeuroses. FOP is associated with progressive and permanent loss of mobility, lower quality of life, and shortened lifespan3-5. Malformation of the great toes and progressive HO are the two hallmark clinical features of classic FOP6,7. Additional skeletal features in patients with FOP may include short thumbs, short broad femoral necks, cervical spine malformations, distal femoral and proximal medial tibial osteochondromas, and early developmental arthropathy8,9. Classical FOP results from a recurrent activating mutation (617G > A; R206H) in the gene encoding a bone morphogenetic protein (BMP type I) known as activin A receptor type I/activin-like kinase 2 (ACVR1/ALK2)10.
Beginning in early childhood, episodic inflammatory pre-osseous lesions, commonly known as flare-ups, involve various soft tissues (eg, aponeuroses, fascia, ligaments, tendons, skeletal muscle). Swelling and pain are the most common early symptoms of flare-ups, but other symptoms, such as stiffness, warmth, decreased movement, changes in mood or behavior, fever, loss of appetite, and lethargy may occur11. While some flare-ups resolve spontaneously without consequences, most lead to HO of soft connective tissues resulting in permanent immobility7,12,13. Various minor and major bodily traumas can stimulate flare-ups, including influenza-like illnesses, use of mandibular block for dental work, intramuscular immunization, muscle fatigue, and blunt muscle trauma from bumps, bruises, and falls3,7. Thus, it is important that medical planning for individuals with FOP includes injury reduction strategies, especially because current treatment relies on palliative care, as there are no definitive medical treatments approved for preventing HO14. While early diagnosis of FOP is important to prevent irreversible harm from typically innocuous procedures, misdiagnosis is common13.
HO occurs episodically, but the disability in patients with FOP is cumulative, leading to immobilization and confinement to a wheelchair commonly before the end of the third decade of life. Therefore, individuals with FOP typically require lifelong assistance to perform activities of daily living7,12,13. The median estimated lifespan of individuals with FOP is 56 years, with the most common cause of death being complications of thoracic insufficiency syndrome4.
The objective of this study was to evaluate the extent to which caregiver support is needed in this patient population. Using the FOP Registry, an international, voluntary effort that records demographic and disease data on patients with FOP15, the findings in this report expand those from a recent report by Pignolo and colleagues describing common symptomology; aides, assistive devices, and adaptations (AADAs); and physical function16.
Methods
FOP Registry
The FOP Registry was launched by the IFOPA with a guiding vision to develop and manage one unified, global, and coordinated registry, allowing the assembly of the most comprehensive data on FOP. The primary goal of the registry is to facilitate greater access to shared data, to enable better monitoring of patient care, to responsively inform clinical trial design, and to foster accelerated development of transformative therapies. The FOP Registry is an ongoing international, voluntary, observational resource that directly captures demographic and disease information from individuals with FOP approximately every six months. The design of the registry has been recently described15.
During the FOP Registry enrollment process, patients provide contact information, confirm FOP diagnosis, provide contacts to local physicians/hospitals where they receive care, and provide electronic acceptance of informed consent information. The FOP Registry includes individuals with classic FOP, other known FOP variants, and unknown genetic status with a clinical diagnosis. As of data collection on September 20, 2018, 299 individuals from 54 countries (approximately 37% of the world's known FOP population-based on IFOPA estimates of 808 individuals worldwide) were enrolled. Thus, this cohort of 299 participants is likely representative of the global FOP community and the 192 participants who answered questions related to caregiving also represent a substantial portion of FOP patients.
Assessment Instruments and Scales
Questions related to caregiver support answered by participants enrolled in the FOP Registry as of September 20, 2018 referred to paid or unpaid FOP-specific care attendants. Registry questions related to caregiver support are shown in Table 1 along with potential responses. The questions are part of the larger registry survey as previously described15 and are included within the section on AADAs. Each participant responded to yes/no and analogue inquiries.
Table 1: Summary of FOP Registry questions to assess caregiver support
|
Question |
Response format |
|
Use of FOP-Specific Care Attendants (Paid or Unpaid) Bathing attendant(s) Part-time home personal care attendant(s) Number of part-time assistants Full-time home personal care attendant(s) Number of full-time assistants Full-time personal school aide |
Yes or No Yes or No Numeric Yes or No Numeric Yes or No |
Statistics
All data were summarized at enrollment for sex and current age group: 0 to <9 years of age, 9 to 15 years of age, >15 years of age, and all ages. Descriptive summaries of categorical outcomes included the number (n) and percent of registry participants. Percentages are based on all participants enrolled with data within each category and age group. Participants who withdrew from the study were excluded. The Mantel-Haenszel Chi-Square test was used to measure the association between patient use of bathing attendants, part-time personal care attendants, and full-time personal care attendants and age group. A chi-squared test was used for comparison of female vs. male patients' need for care attendants. A Cochran-Mantel-Haenszel (CMH) General Association controlling for age group was used to measure the overall association in the percent of respondents between the number of part- or full-time home personal care attendants.
Results
Patient Demographics and Diagnosis
Of the 299 participants enrolled in the FOP Registry as of September 20, 2018, a total of 192 participants answered questions related to caregiving. Of these participants, 113 (58.9%) were female and 79 (41.1%) were male.
Caregiving Support
Overall, 58 (30.2%) of the 192 registry participants who responded to questions on caregiving noted the use of one or more part-time home personal attendants, and 51 (26.6%) noted the use of one or more full-time personal care attendant(s) (Table 2). The use of part-time attendants was more common in male patients compared to female patients (34.2% vs. 27.4%; p=0.3166), while use of full-time attendants (20.3% vs 31.0%, respectively, p= 0.0979) was less common, however neither of these differences reached statistical significance. The need for caregiving increases with age for FOP patients (Figure 1). In the 0 to <9 years group, 21.4% (6 of 28) utilize a bathing attendant. The percentage increases to 45.2% (19 of 42) in the 9 to 15 years group and to 51.6% (63 of 122) in the group of FOP patients >15 years of age. The association between the need for bathing attendants and age is statistically significant (p=0.0063) such that the requirement for bathing attendants increases with age. Similarly, statistically significant associations are noted for both part-time and full-time home personal care attendants (p=0.0408 and 0.0263, respectively). In the 0 to <9 years group, 14.3% (4 of 28) utilize a part-time home personal care attendant, and the percentage increases to 28.6% (12 of 42) in the 9 to 15 years of age group and to 34.4% (42 of 122) in the group >15 years of age. In the 0 to <9 years of age group, 14.3% (4 of 28) utilize a full-time home personal care attendant. The percentage increases to 19.0% (8 of 42) in the 9 to 15 years of age group and to 32.0% (39 of 122) in the >15 years of age group.
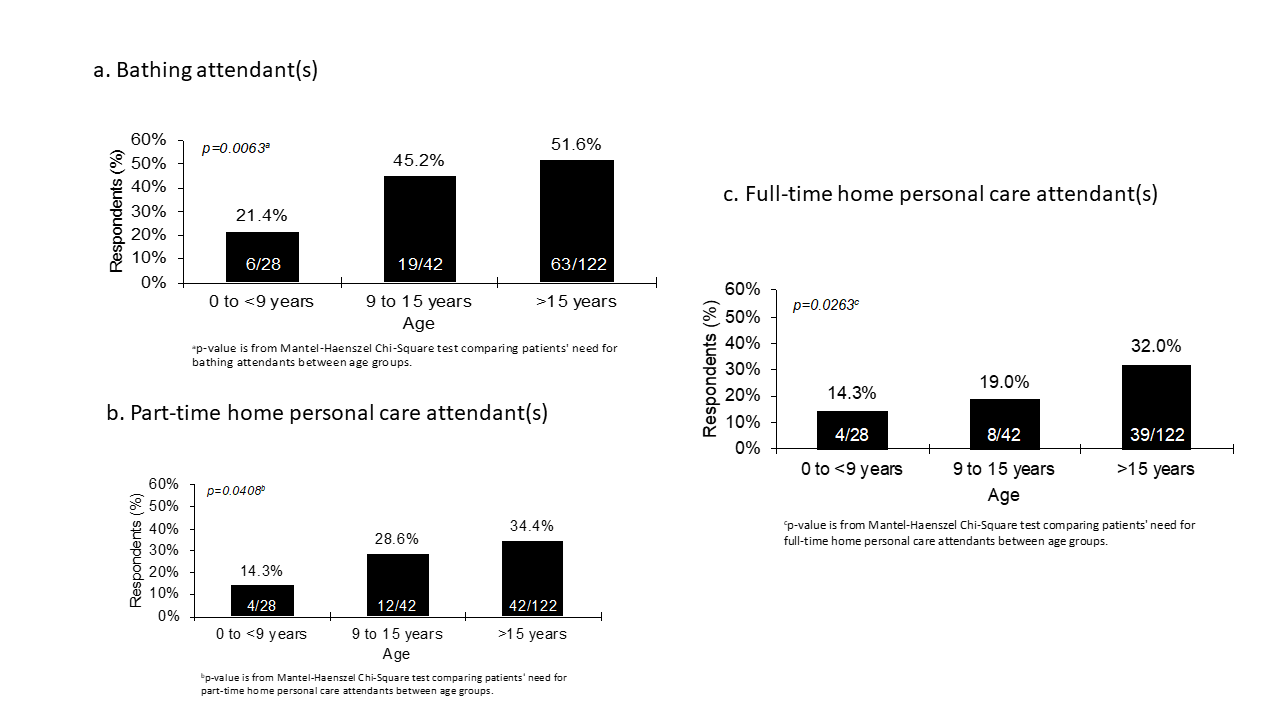
Figure 1: The Need for Caregiving in FOP
The need for caregiving in FOP increases with age. The percentage of registry responders that require (a) bathing attendant(s), (b) part-time home personal care attendant(s), or (c) full-time home personal care attendant(s) increases significantly with age.
Table 2: Caregiver support measured as the need for patient care attendants
|
|
Female (n=113) |
Male (n=79) |
Total (n=192) |
p-valuea |
|
Part-time home personal attendant(s), n (%) |
31 (27.4%) |
27 (34.2%) |
58 (30.2%) |
0.3166 |
|
Full-time home personal attendant(s), n (%) |
35 (31.0%) |
16 (20.3%) |
51 (26.6%) |
0.0979 |
a p-value is from Chi-square test comparing patients' need for care attendants between female vs. male at enrollment.
Number of Personal Care Attendants
The use of full-time home personal care attendants increases with age among patients with FOP and a larger percentage of FOP patients who require ≥2 attendants are in the older age groups (Figure 2a). However, across age groups, patients are most likely to use a single full-time personal care attendant, and increasingly fewer participants reported the use of additional full-time care attendants (2, 3, ≥4; p= <0.0001). In the 0 to <9 years group, 3.6% (1 of 28) utilize 1 full-time home personal care attendant, 17.9% (5 of 28) utilize 2, 3.6% (1 of 28) utilize 3, and no respondents in this group utilize ≥4. Among the 9 to 15 years group, 19.0% (8 of 42) of FOP patients utilize 1 full-time home personal care attendant, 4.8% (2 of 42) utilize 2, 9.5% (4 of 42) utilize 3, and 2.4% (1 of 42) utilize ≥4. Among the >15 years group, 18.0% (22 of 122) of FOP patients utilize 1 full-time home personal care attendant, 9.0% (11 of 122) utilize 2, 4.1% (5 of 122) utilize 3, and 2.5% (3 of 122) utilize ≥4. The overall use of part-time home personal care attendants is similar to that for full-time home personal care attendants within each age group (Figure 2b) and the significantly greater likelihood that participants have 1 part-time personal care attendant persists (p<0.0001).
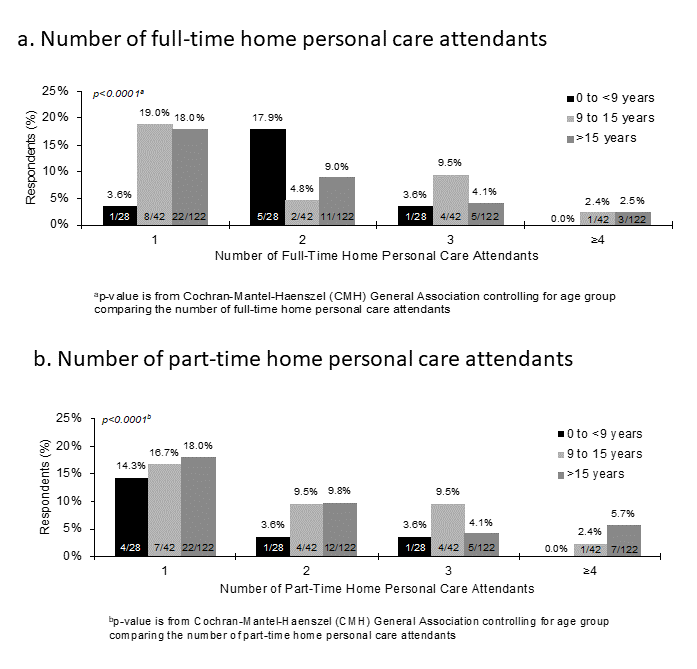
Figure 2: Care attendants stratified by patient age in FOP
Number of (a) full-time and (b) part-time home personal care attendants stratified by patient age in FOP. Across age groups, patients are most likely to use a single full-time or part-time personal care attendant, and increasingly fewer participants reported the use of additional full-time or part-time care attendants (2, 3, ≥4; p= <0.0001).
Use of Personal School Aides
Personal school aide support (mainly for patient safety) is often used during the formative years in FOP (Figure 3), though is inversely correlated with age group (p<0.0001) for participants overall, with the rate in usage of school aides decreases with age. There appears to be a possible gender difference in utilization of personal school aides, with 58.8% of females between the ages of 9 and 15 utilizing personal school aides compared with 32.0% of males. The use of school aides appears low in the >15 years group due to the inclusion of individuals who have likely completed their final year of schooling, including college or university studies.
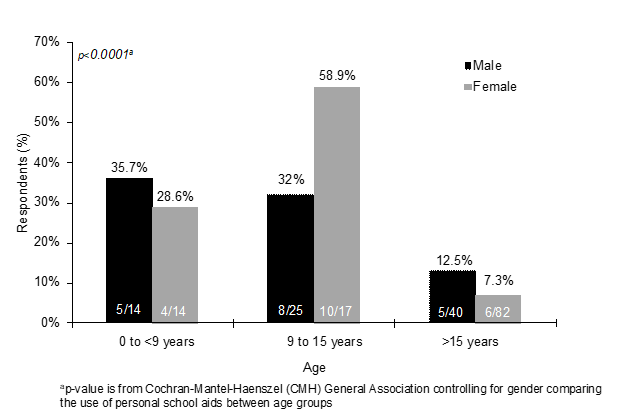
Figure 3: Use of personal school aides by age group and gender
There is a strong overall correlation in the usage of personal school aides among the age groups while adjusting for gender effects. The rate in usage of school aides decreases with age (p=<0.0001).
Discussion
This is the first report to describe and categorize caregiver support in FOP. While the caregiver support is thought to be high for patients with FOP, the true impact has not been quantified, and to the knowledge of the authors, there are no comparable studies that evaluate caregiver support for other conditions which affect musculoskeletal function in a similar way.
In the present study, we used data from the FOP Registry, which included 299 patients at the time of data collection, representing global participation from 54 countries and about 37% of the world’s known FOP population. More than half of FOP Registry participants responded to questions related to caregiving support, allowing the analysis of not only the utilization of caregiving support, but also how this utilization evolves over time. As FOP patients progress through adolescence and teenage years, the requirement for bathing attendants and part- or full-time home personal care attendants significantly increases. In addition, the number of part- or full-time attendants also significantly increases with age. In FOP patients >15 years of age, the percentages of individuals utilizing ≥1 part-time or full-time attendants both exceeded 30%.
In 2017, Kaplan and colleagues published a cumulative analogue joint involvement scale (CAJIS) for FOP, which is a simple, easy-to-administer scale to assess functional mobility in FOP17. The CAJIS score and modified CAJIS score are highly correlated with patient-reported mobility assessments, and the modified CAJIS score is correlated with the total mean score for use of AADAs16,18. AADA use increases with age group, a pattern that is reflected in the utilization of part-time and full-time care observed in this study.
In FOP, mobility changes tend to be episodic and regional. Immobility most often occurs first in the neck and trunk, followed by the upper limbs and finally by the lower limbs. In a natural history study of FOP, Pignolo and colleagues published results from a 78-question survey of 685 patients with FOP in 48 countries, including the median age-at-onset of impairment of body regions11. By the age of 9 years, body regions that are typically affected include the neck, upper back, lower back, shoulder, chest, and abdomen. Between the ages of 9 and 15 years, the elbows, hips, and knees, are often affected. Between 15 to 18 years of age, typically affected joints include the ankles, wrists, fingers, feet, and jaw.
As the number of regions affected by HO increases, overall mobility decreases, including complete ankyloses of joints, resulting in cumulative functional impairment over time19. Thus, much of the reported caregiver support needed for patients as they move into adulthood is already in place in the 9 to 15 year-old group, as demonstrated by the results of this study (Figure 1).
A recent study by Pignolo and colleagues reported on the use of AADAs from the same FOP Registry on which the present study is based16. AADAs may include FOP-specific care attendants; eating and personal care tools; bathroom and bedroom aides and devices; adaptations for home; school, and work environments; adaptations for technology, sports, and recreation; and medical therapies for daily living. The use of AADAs increased with age, with the group of participants 9 to 15 years of age having a median AADA use of more than three times that of the 0 to < 9 year-old group; the > 15 year old group had more than six times the median AADA use compared to the 0 to < 9 year-old group. AADA usage appears to be correlated with higher PROMIS global health scores (i.e., better quality of life) in males, whereas not having to use an AADA (with the exception of home ramps) was associated with higher PROMIS global health scores in females. These differences were attributed to the higher number of females in the registry, fewer of whom are using AADAs than males. Alternatively, the findings could also suggest that gender plays a role in the perception of quality of life related to AADAs. Of note, 43.2% of participants indicated that they did not have at least one part-time caregiver, which may indicate that for some patients, the use of AADAs and a modified home environment offers sufficient support or potentially reduces the need for paid caregivers.
The need for support from school aides peaked between 9 and 15 years of age, as disability is increasing, and suggested a gender difference of greater need among females in the age group between 9 and 15 years. However, the reason for this is unclear and requires further investigation. Though the apparent sex-based difference in school aides observed between 9 and 15 years of age may be of interest, multiple studies to date indicate that sex is not a variable influencing disease progression in FOP. Furthermore, it is not clear which self-reported measures of function are likely to track specifically with differential use of school aides, or to our knowledge, are validated as such. Finally, there is no way to account for individual or gender-related methods of learning that might influence the propensity toward using any or type of school aides. While the use of school aides decreased in the group >15 years of age relative to the younger age groups, it is important to note that much of this cohort is past high school age and thus would either not utilize school-based aides or may vary with regards to whether or not they consider assistance for college or university learning to be school-based assistance.
Limitations
As with all studies of observational registries, limitations exist20,21. Because enrollment into registries is voluntary, data may be missing, inaccurate, or incomplete. In addition, participant subjectivity and loss to follow-up may limit the possible scope of analysis or compromise the validity of results. It should be noted that the FOP Registry is centralized and curated at one site, unlike other registries that lack standardized assessment, data collection, or the requirement of multiple sites15. Another limitation of this study is that many caregivers of children with chronic diseases are parents; however, the parent(s) may not view themselves, siblings, or other relatives as part-time or full-time care attendants. Therefore, the actual dependency on caregiving among FOP patients is likely underestimated due to the tendency for parents to not consider themselves a caregiver when answering registry questions. In addition, though the number of part-time and full-time caregivers provides some picture of time needed for caregiving, measures of caregiver support should ideally also include a more granular view of time spent on caregiving activities. Unfortunately, information on hours spent is not available through FOP Registry data, and hence not evaluated.
Importantly, the need for caregiving is not equivalent to access to caregiving. Globally and nationally, coverage of caregiving services can vary, resulting in a lack of access for some families despite need. The topic of how access to needed caregiver support, or lack thereof, affects social, economic, and psychological aspects of patient life will be an important element of future work in FOP. Despite these limitations, analysis of the FOP Registry data provides valuable descriptive data from which testable hypotheses can be generated.
Conclusion
The findings here suggest that caregiver support in FOP is high in terms of the amount of support needed to care for individuals with FOP. Clinically, studies such as this aid healthcare providers and families in anticipating and preparing for future care needs through assistive devices or practices (e.g., canes, wheelchairs, care attendants), the implementation of which can facilitate mobility and activities of daily living as well as preserve independence.
Conflict of Interest
The authors declare no conflicts of interest related to the work described in this paper.
Acknowledgments
This work was supported by the IFOPA, the Radiant Hope Foundation (RJP, MA), the Robert and Arlene Kogod Professorship (RJP) and the Isaac & Rose Nassau Professorship of Orthopaedic Molecular Medicine (FSK). The FOP Registry has been supported by The Radiant Hope Foundation, Blueprint Medicines, Ipsen, and Regeneron Pharmaceuticals. The authors would like to thank Ginny Vachon, PhD and Cecelia Shertz Wall of Principal Medvantage Writing, LLC in Atlanta, Ga, USA for editorial support. Funding for editorial support by the IFOPA.
References
- Baujat G, Choquet R, Bouee S, et al. Prevalence of fibrodysplasia ossificans progressiva (FOP) in France: an estimate based on a record linkage of two national databases. Orphanet J Rare Dis. 2017; 12(1): 123.
- Liljesthröm M, Pignolo RJ, Kaplan FS. Epidemiology of the global fibrodysplasia ossificans progressiva (FOP) community. J Rare Dis Res Treat. 2020; 5(2): 31-36.
- Pignolo RJ, Shore EM, Kaplan FS. Fibrodysplasia ossificans progressiva: clinical and genetic aspects. Orphanet J Rare Dis. 2011; 6: 80.
- Kaplan FS, Zasloff MA, Kitterman JA, et al. Early mortality and cardiorespiratory failure in patients with fibrodysplasia ossificans progressiva. J Bone Joint Surg Am. 2010; 92(3): 686-691.
- Ortiz-Agapito F, Colmenares-Bonilla D. Quality of life of patients with fibrodysplasia ossificans progressiva. J Child Orthop. 2015; 9(6): 489-493.
- Bravenboer N, Micha D, Triffit JT, et al. Clinical utility gene card for: Fibrodysplasia ossificans progressiva. Eur J Hum Genet. 2015; 23(10): 1431.
- Pignolo RJ, Shore EM, Kaplan FS. Fibrodysplasia ossificans progressiva: diagnosis, management, and therapeutic horizons. Pediatr Endocrinol Rev. 2013; 10 Suppl 2: 437-448.
- Kaplan FS, Xu M, Seemann P, et al. Classic and atypical fibrodysplasia ossificans progressiva (FOP) phenotypes are caused by mutations in the bone morphogenetic protein (BMP) type I receptor ACVR1. Hum Mutat. 2009; 30(3): 379-390.
- Towler OW, Shore EM, Kaplan FS. Skeletal malformations and developmental arthropathy in individuals who have fibrodysplasia ossificans progressiva. Bone. 2020; 130: 115116.
- Shore EM, Xu M, Feldman GJ, et al. A recurrent mutation in the BMP type I receptor ACVR1 causes inherited and sporadic fibrodysplasia ossificans progressiva. Nat Genet. 2006; 38(5): 525-527.
- Pignolo RJ, Bedford-Gay C, Liljesthrom M, et al. The natural history of flare-ups in fibrodysplasia ossificans progressiva (FOP): a comprehensive global assessment. J Bone Miner Res. 2016; 31(3): 650-656.
- Kaplan FS, Xu M, Glaser DL, et al. Early diagnosis of fibrodysplasia ossificans progressiva. Pediatrics. 2008; 121(5): e1295-1300.
- Kitterman JA, Kantanie S, Rocke DM, et al. Iatrogenic harm caused by diagnostic errors in fibrodysplasia ossificans progressiva. Pediatrics. 2005; 116(5): e654-661.
- The International Clinical Council on FOP (ICC) and Consultants. The medical management of fibrodysplasia ossificans progressiva: Current treatment considerations. May 2021. Available at: http://www.iccfop.org/dvlp/wp-content/uploads/2021/04/GUIDELINES-Apr-2021.pdf
- Mantick N, Bachman E, Baujat G, et al. The FOP Connection Registry: Design of an international patient-sponsored registry for Fibrodysplasia Ossificans Progressiva. Bone. 2018; 109: 285-290.
- Pignolo RJ, Cheung K, Kile S, et al. Self-reported baseline phenotypes from the International Fibrodysplasia Ossificans Progressiva (FOP) Association Global Registry. Bone. 2020; 134: 115274.
- Kaplan FS, Al Mukaddam M, Pignolo RJ. A cumulative analogue joint involvement scale (CAJIS) for fibrodysplasia ossificans progressiva (FOP). Bone. 2017; 101: 123-128.
- Kaplan FS, Al Mukaddam M, Pignolo RJ. Longitudinal patient-reported mobility assessment in fibrodysplasia ossificans progressiva (FOP). Bone. 2018; 109: 158-161.
- Pignolo RJ, Baujat G, Brown MA, et al. Natural history of fibrodysplasia ossificans progressiva: cross-sectional analysis of annotated baseline phenotypes. Orphanet J Rare Dis. 2019; 14(1): 98.
- Temple R. Problems in the use of large data sets to assess effectiveness. Int J Technol Assess Health Care. 1990; 6(2): 211-219.
- Canto JG, Kiefe CI, Williams OD, et al. Comparison of outcomes research with clinical trials using preexisting data. Am J Cardiol. 1999; 84(8): 923-927.
